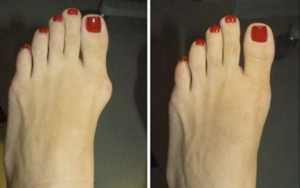
Bunions (Hallux Valgus)
A bunion is an abnormal bump that forms on the joint at the base of your big toe. It’s a bone deformity caused by your big toe pushing up against your other toes, which forces the big toe joint in the opposite direction. Bunions can be very painful, especially around the outside of the base of your big toe, and are best treated by a specialist surgeon or podiatrist performing bunion surgery.
BUNION SURGERY
Am I Ready for Bunion surgery?
Only you and a Specialist Orthopaedic surgeon can decide on when is the right time. Being educated and counselled on this by your orthopaedic surgeon at Surrey Orthopaedic Clinic will help. Many people delay treatment due to fear, misinformation and a lack of awareness of their options. Often, many of these same people wish they had it done sooner.
At the Surrey Orthopaedic Clinic, we use the most advanced technology and techniques using only the best quality products on the market to revolutionise recovery rates and maintain excellent outcomes. Foot and ankle surgery is related to need, not age.
What should I Expect from Bunion surgery?
Surgery for bunions involves more than just simply shaving the big toe bony bump (protrusion). It typically requires the deviated bones to be structurally realigned. Mild bunions are corrected with bone cuts close to the big toe joint. Large bunions typically need a more “involved” bone cut or a fusion procedure to completely realign the structural problem. It takes approximately six weeks for the bones to mend in the corrected position.
Is Bunion Surgery Very Painful?
Bunion surgery is not particularly “more” painful than other surgery. Foot surgery, in general, can lend itself to increased pain post-operatively because the foot is below the level of the heart and blood can rush to the area, causing a throbbing feeling. Also, the foot does not have much soft tissue padding surrounding the bones, so moderate postoperative swelling can aggravate the nerves, causing pain. Most patients find the postoperative discomfort is tolerable with pain medication.
Can Bunions Come Back Even After Surgery?
The majority of patients are satisfied with their outcome after bunion surgery. Recurrence is possible, but not particularly likely. And, return of a bunion is not necessarily a complication, but something that can happen over time. Some patients have excessive motion in the foot that may predispose them to recurrence. Another possible reason for recurrence occurs when a procedure that was performed did not best suit the severity of the particular bunion…so it’s important to have the surgery tailored for your particular bunion.
Will I need to have a Plaster Cast and Crutches after Bunion Surgery?
Modern techniques have allowed surgeons to mobilise patients quicker. Recent technological advances in medical implant devices have also helped our surgeons modify their techniques to get patients moving quicker.
Mild bunions typically involve walking in a surgical shoe for six weeks. Surgeons consider casting with crutches with larger bunions because setting the bones can be more complex.
How Long Will I need off Work after Bunion Surgery?
For desk-based jobs and depending on the type of surgery performed, it is possible to perform some work from home one week after surgery. If possible it is ideal to take off 2 weeks to minimise swelling and maximise rehabilitation time with the physiotherapists.
Jobs that require excessive walking, standing and physical activity may require a medical leave of absence which can be up to two months depending on healing and job requirements. Getting around can be difficult and driving may be off limits if you have your right foot operated on and/or drive a manual.
Is Surgery only for painful Bunions? Will my Bunions get better if I leave them well alone?
The concern with surgically correcting a non-painful bunion is that the surgery can result in longstanding post-operative pain that may not have been there prior. However, people do have surgery for non-painful bunions if the bunion interferes with activity, continues to become larger, or if they have difficulty wearing certain shoes and/or if the bunion is simply unsightly. A Bunion is not just a soft tissue problem but a bone and joint deformity with muscle imbalance. Without surgery, the deformity will NEVER self-correct. Non-surgical treatments allow function and provide some pain relief but the bunions will always be persistent.
What Are the Scars like after Bunion Surgery?
Surgical healing is part of the process with any surgery, and bunion surgery is no different. Incisions are minimal, and surgical approaches are used to hide surgical scars. Bunion incisions are either located on the top of the foot or on the side of the foot, and technique varies based on surgeon. At Surrey Orthopaedic Clinic, our experienced specialists keep scaring to a minimum.
What can I expect on the day of Bunion surgery?
On the day of your operation you will be met at reception by hospital staff and taken to your own room. Unlike the NHS, where we supervise but may not perform every operation on every patient, privately only one of our Specialists such as Mr Chana, Mr Michael or Mr Masucci will see you prior to the procedure in your room and then perform the procedure personally.
After your operation you may feel drowsy but will feel little or no pain. We will see that you are well in the recovery suite of the operating theatre and in your room later. We will telephone your partner or next of kin to let them know that all went well.
Will I need an anaesthetic (to be put to sleep) for Bunion Surgery or is it done under a “local”?
The operation is performed under a general anaesthetic combined with a local injection (given whilst you are asleep) to minimise pain after the operation.
How long does the Bunion Operation take?
Typically 45 to 90 minutes.
How long is the Recovery after Bunion Surgery?
Most Foot and Ankle surgery is done as a Day Case. That means you come in for the operation and go home the same day. Unless the surgery is performed later in the afternoon or early evening when we advise a 1 night to stay to allow time to be spent with the physiotherapist before discharge.
You will be seen by your specialist and a physiotherapist who will teach you how to walk using crutches and how to use the surgical boot or shoe that may be necessary after your operation.
What is the Rehab after Bunion Surgery?
After surgery, you will be most likely be walking with crutches for two weeks and then seen by your specialist at the Surrey Orthopaedic Clinic, where we will tailor your recovery to suit your personal circumstances and needs. The most important thing is that you feel as little pain as possible after the operation and make a safe recovery according to the plan agreed.
After surgery, you will need to keep the foot elevated at eye level for 40 minutes out of every waking hour for the first week and can reduce this by ten minutes a week thereafter. This is to prevent swelling which can hinder wound healing. Whilst elevating the foot you must keep moving the foot and ankle up and down to contract the calf muscle which act as a pump to keep the blood flowing through the leg which prevents a clot. Do this for 5 minutes every half an hour or 30 seconds every five minutes.
Rehabilitation programmes are tailor-made for each individual based on the patients needs. Typically rehabilitation with physiotherapists lasts 6-12 months.
When will I be able to get back to playing sports after Bunion Surgery?
Generally between 8-12 months depending on which sports. Higher-level athletes with more intensive rehabilitation may get back closer to 6 months.
Can I drive after Bunion Surgery?
Driving may be resumed a few weeks after surgery, although usually you are given the go ahead once seen at the clinic around the 6-week mark. If the surgery was performed on your right side, your surgeon may ask you to wait longer than if you had surgery on the left side, assuming you drive a car with automatic transmission. In any case you must be able to move the leg easily from the accelerator to the brake, and make a safe emergency stop before driving. This time typically varies from 4 to 8 weeks depending on multiple factors. Always inform your insurance company before going back to driving once given the all clear by your surgeon
Complications of Bunion surgery
All surgical procedures have the potential for complications and foot surgery is no different in this respect.
Major complications include:
-
- Stiffness & swelling: Initially the foot will be very swollen and needs elevating. The swelling will disperse over weeks/months but may still be apparent at 6-9 months. Often shoes will remain tight for 8-12 weeks. The toe will be stiff but will usually regain its original movement.
- Infection: There is always a risk of infection with surgery. You will be given 1 dose of intravenous antibiotics during surgery. The best way to reduce the chance of acquiring an infection is to keep the foot elevated for 10 days. If you smoke, stopping during the healing phase will dramatically reduce your chances of infection or wound healing problems. If there is an infection it normally resolves with a course of oral antibiotics.
- Nerve damage: A nerve supplying the side of the toe lies beneath the incision, and this is at risk of damage. Usually it is only bruised and will recover. If the damage is permanent, there will be a small patch of numbness. This does not normally cause any disability.
- Under correction: Occasionally, the deformity of the toe is not fully corrected. This is more common in severe cases. This is rarely problematic and requiring of further surgery.
- Over correction: Very rarely the toe can be over-straightened so that it angles away from the foot (hallux varus). This usually requires further surgery.
- Avascular Necrosis: This is where the blood supply to the bone is disrupted, leading to the bone tissue dying and collapsing, and the joint surfaces being damaged. This can lead to arthritis (pain and stiffness), which may require further surgery.
We will also discuss Deep Vein Thrombosis (blood clot in your deep veins in the leg) prophylaxis in the clinic and we would recommend bilateral TED stockings and immediate full mobility weight bearing in order to keep the blood flowing through the leg and this means you have achieved full mobility immediately after surgery. Mechanical prophylaxis would be indicated but you may require pharmaceutical measures balancing the risk of bleeding against the risks of blood clots being minimised. A risk of using chemical injections or a tablet to thin the blood (Clexane, Fragmin or Rivaroxaban, all forms of Heparin) is that the blood becomes too thin and forms a haematoma or collection of blood around the joint. This may require a further operation to wash out the blood and prevent an infection. This can happen in 1 out of 200 cases.
If an infection takes hold, this can lead to further surgery and even amputation in 1 in 1000 cases. The other thing to keep in mind is that up to 1 in 500 of people using Clexane or Fragmin can develop Heparin Induced Thrombocytopenia (HIT). This is a condition where the blood platelets become consumed due to the blood thinning injections. This can be an emergency where you need to be admitted and treated for generalised clots within the body, which can lead to multi-organ failure in severe cases as well as a platelet transfusion. A blood test to measure your levels will usually be performed to check your platelet levels are fine. Your surgeon will discuss your risk profile with you and a shared decision will be made prior to surgery about how to tackle the problem preventing a deep vein thrombosis and its complications.
Each Specialist at the Surrey Orthopaedic Clinic will keep accurate records of their own data for the risks above. Please do not hesitate to ask about this during your visit. Our complication numbers are amongst the lowest in the country.
As you might imagine, training and experience are very important in ensuring a good outcome for patients. We are delighted to say that our patients are extremely satisfied with the care and their outcomes. We are a recognised specialist group in this field and have pioneered new reconstruction techniques and recovery protocols to world-class standards. This is reflected both in our results as well as in our role training junior surgeons and fellow consultants how to carry out the procedures as part of our NHS commitments.
Surrey Orthopaedic Clinic Foot & Ankle Specialists:





